“It seems so simple,” began Hamid Shokoohi, M.D., M.P.H. ’06, associate professor of emergency medicine at the George Washington University (GW) School of Medicine and Health Sciences (SMHS). “A patient with multiple injuries as a result of a car accident would get attention if she were in the heart of the largest hospital in a capital city. But that was not the story of a patient we saw on the last day of my trip to Malawi.”
When Shokoohi hurried to the patient, what he and his colleagues found was “shocking: a 24-year-old female with multiple injuries, left alone in the radiology hallway and awaiting a chest X-ray, with a nervous husband at her bedside. This patient could have easily matched the highest level of trauma code in any trauma center in the United States.”
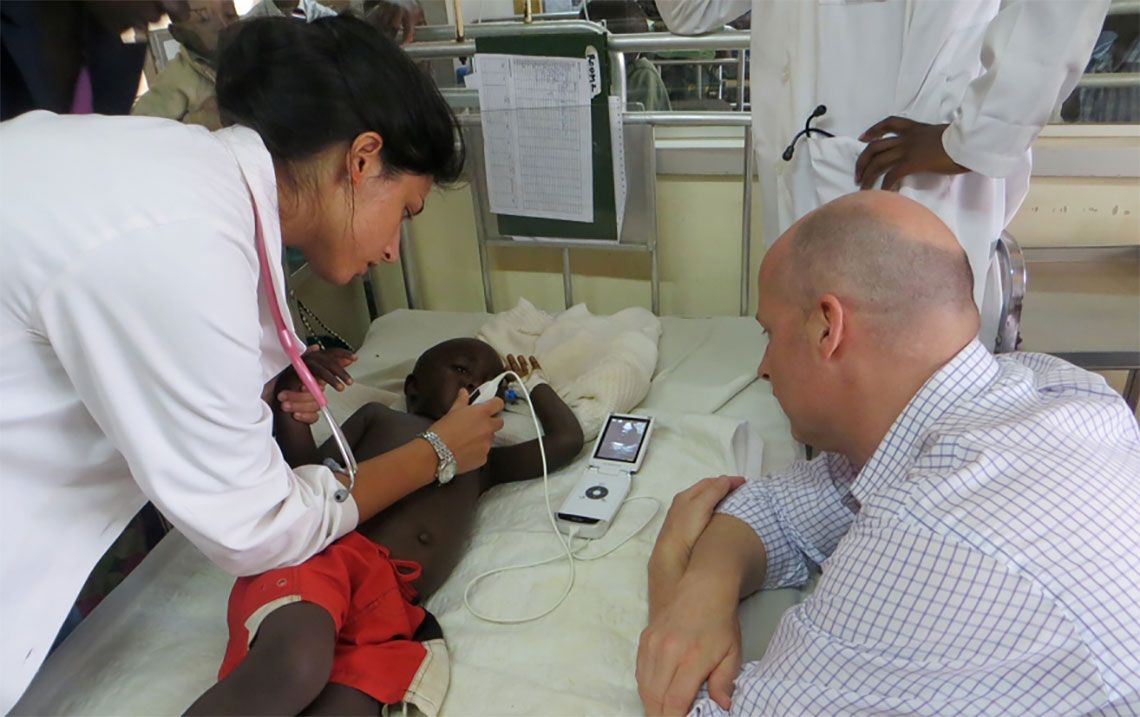
Shokoohi pulled his Vscan, a handheld ultrasound device, from his pocket and conducted a quick chest and abdominal scan; he found significant intra-abdominal bleeding with clotting and possible splenic rupture. Shokoohi shared the images with a local surgeon and a volunteer surgeon, and they rushed the patient into the operating room for an emergency laparotomy. She survived.
Shokoohi’s anecdote – one of many that both he and his colleague, Keith Boniface, M.D., chief of ultrasonography and associate professor of emergency medicine at SMHS, share – highlights the health disparity between the United States and developing countries.
“Opportunities for a healthy life are not equally distributed across the globe,” Boniface said.
In an effort to balance the scales, GW joined forces with Global Health Service Partnership (GHSP), a collaboration between the Peace Corps, the President’s Emergency Plan for AIDS Relief, and non-profit Seed Global Health. GW’s role, explained Jim Scott, M.D., professor of emergency medicine at SMHS and senior advisor for medical education at Seed Global Health, is organizing the program participants’ medical orientation and training in collaboration with the Peace Corps. During a two-week intensive session in Washington, D.C., the mix of volunteer doctors and nurses learn about infectious diseases, safety and security, and the culture and health conditions of the three participating countries, Malawi, Tanzania, and Uganda. The group then travels to Africa, where they receive additional training before assuming year-long faculty roles in medical and nursing schools. The GHSP program is now in its third year of sending volunteers abroad.
Since 2014, the GE Foundation has partnered with Seed Global Health to equip GHSP volunteers with Vscan devices for diagnostic use and training purposes. GW, in response, has incorporated additional ultrasound training for the volunteers.
“We felt that we needed to get the volunteers some hands-on training, both in the equipment and in the whole field of ultrasound that was new to them,” said Scott, a former Peace Corps volunteer. “We’re finding that ultrasound is really important.”
Scott turned to “the smartest point-of-care ultrasound guys I know,” Shokoohi and Boniface. Twice, the doctors led training in the United States before heading to Africa to complete an additional round of training. It was there, they say, their scope of experience widened.
“My experience with GHSP volunteers during these trips with local professionals was absolutely profound,” Shokoohi said.
As the doctors explained, the Vscan made an immediate impression on diagnostics. As a small device that runs on battery power, the scanner allows medical facilities to bypass the challenges of expensive, bulky equipment that requires maintenance and steady electricity.
“This device is not the most advanced, but it’s the most available, accessible device for the providers,” Shokoohi explained.
Boniface agreed: “When you look at the price on this small, handheld device, comparing that to the impact it can have, it’s really perfect for that health care setting. These machines are tiny. They break, you stick them in a box, you mail them back, and they fix it and return it, or they give you a new one.”
While the Vscan doesn’t provide the comprehensive imaging of a larger machine, its convenience allows medical workers to speedily attend to patients. In the two visits Shokoohi and Boniface made to Africa, they witnessed – and were part of – the pivotal change the Vscan provided, particularly with HIV- and tuberculosis-related diagnoses.
“The 9-year-old with HIV and extreme shortness of breath?” Boniface offered as an example. “Is it pneumonia? Fluid building up around the lungs? Heart failure? Life-threatening compression of the heart inside the pericardial sac by a collection of fluid? With ultrasound providing the definitive diagnosis, the sometimes drastic steps needed to treat each individual condition can be taken with confidence.”
Shokoohi and Boniface both say that their time in Africa has shaped their view of medicine, particularly when it comes to the lengths the local doctors and nurses go in caring for their patients.
“There is nothing comparable to being physically in Malawi and Tanzania to experience what the locals do to help their own people,” Shokoohi said. “Their positive attitudes and their friendly characters are infectious.”
GHSP may expand to additional countries and disciplines in future years, said Scott and Fitzhugh Mullan, M.D., Murdock Head Professor of Medicine and Health Policy at the Milken Institute for Public Health at GW and founding board chair and senior advisor for Seed Global Health. The expansion will likely allow the education and training GW and its professors provide for their African counterparts and the volunteers to spread.
“I firmly believe that by training the health care leaders of tomorrow, we can positively impact health care in a sustainable manner,” Boniface said. “With a continuing mentoring and teaching presence, the number of lives touched by the program can grow exponentially.”


