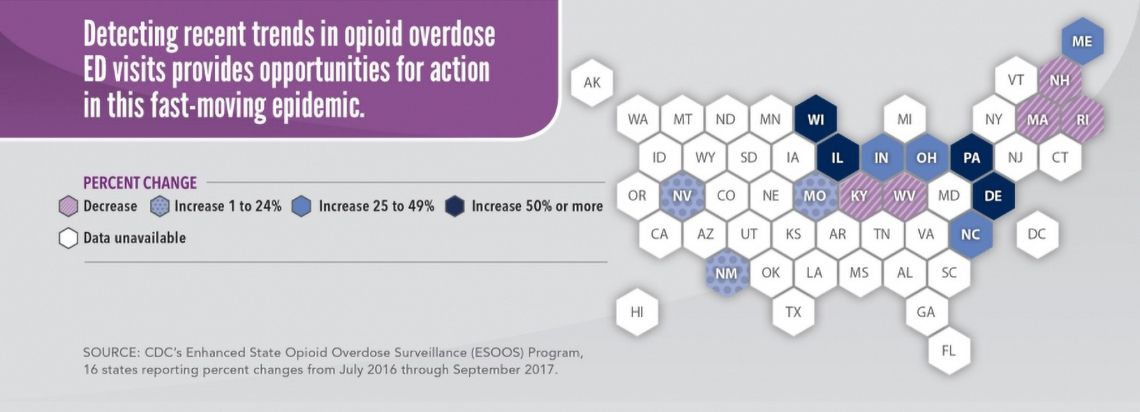
The emergency department has become a prominent battle-ground for our nation’s opioid epidemic. The CDC estimates that between July 2016 and September 2017 over 140,000 patients visited an ER for overdose nationwide. At a time where a staggering 4 out of 5 new heroin users started out misusing prescription painkillers1 often prescribed by a by a physician for acute pain or injury, emergency room physicians around the country are finding themselves on the forefront of a deadly crisis that they helped create.
While emergency room based interventions for opioids focus on issues ranging from overdose prevention to medication assisted therapy, many experts believe that the most effective solution lies on changing the way opioids are prescribed in the first place. Such was the thinking of Mark Rosenberg, DO, Chairman of Emergency Medicine for St. Joseph's Healthcare System in Paterson in New Jersey who launched an innovative alternative to opioids (ALTO) program in January 2016. The aim of the program was to limit the use of opioids when possible and to provide alternative protocols for pain management such as non-opioids pain medications, trigger point injections, nitrous oxide, and ultrasound guided nerve blocks.2
Rosenberg began by conducting an exhaustive literature review of all pain articles worldwide in which he looked at most common complaints in the ED as well as best practices for non-opioid treatment. From this, he formalized non-opioid treatment protocols for the top five most common diagnosis which included headache, long bone fractures, kidney stones, back pain and other musculoskeletal pain.
In the first five months of ALTO, the ED successfully reduced opioid prescription in the ED by 38%, treating 500 acute pain patients with non-opioid protocols. At the completion of the first year of the program they successfully reduced opioid prescription in the ED by 57%.3 That same year St. Joseph’s ALTO program won the Urgent Matters Emergency Care Innovation of the year award. As of May of 2018, Rosenberg reported that the reduction in Emergency Department opioid prescriptions had jumped to 82%.4
In 2017 the Colorado Hospital Association (CHA) developed the Colorado Opioid Safety pilot, an ALTO based study conducted in ten hospital emergency departments over the course of six months. The participating sites reached an average of 36% reduction of opioid administration during these months. Based on the success of this pilot the CHA launched the Colorado ALTO project which required ALTO to be implemented in all hospital EDs across the state.5
In June of 2018 the ALTO act, a bill with the goal of expanding the implementation of ALTO and similar programs was one of 25 opioid related pieces of legislation to pass through congress. The ALTO act requires the department of health and human services to carry out a three year program that awards grants to hospitals and emergency departments in order to study, develop, implement or enhance alternative pain management protocols aimed at limiting the use of opioids in the Emergency Department.6
Reference:
- Jones, C. M. (2013). Heroin use and heroin use risk behaviors among nonmedical users of prescription opioid pain relievers – United States, 2002–2004 and 2008–2010. Drug and Alcohol Dependence, 132(1), 95–100. https://doi.org/10.1016/j.drugalcdep.2013.01.007
- Hoffman, Jan. “An E.R. Kicks the Habit of Opioids for Pain.” The New York Times , 10 June 2016.
- Rosenberg , Mark. “ALTO Program .” American Hospital Association , June 2016, https://www.aha.org/system/files/content/16/16behavhealthcaseex-stjoseph....
- Congress looks to St. Joseph's ALTO® as National Opioid Solution. (n.d.). Retrieved December 19, 2018, from https://www.stjosephshealth.org/newsroom/in-the-news/item/1924-congressi...
- “Colorado ALTO Project.” Colorado Hospital Association, https://cha.com/quality-patient-safety/opioid-safety-updates/colorado-al....
- Pascrell, B. (2018, June 13). H.R.5197 - 115th Congress (2017-2018): ALTO Act [webpage]. Retrieved December 18, 2018, from https://www.congress.gov/bill/115th-congress/house-bill/5197
Rebecca Siegel, is a research fellow in the GWU Department of Emergency Medicine and a medical student at Ben Gurion University in Israel.