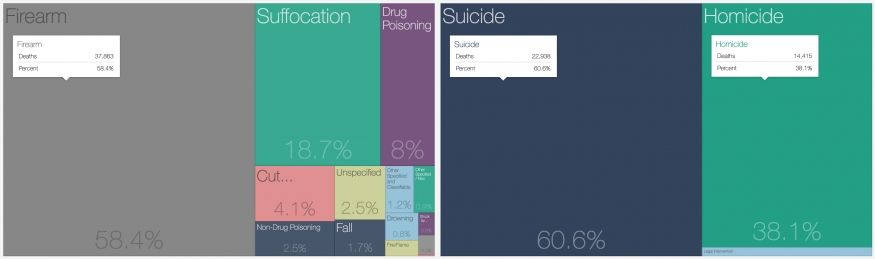
Background
In 2016, there were a total of 63,979 intentional injury deaths in the United States1. Of these, 37,353 (58%) involved a firearm: 22,938 (36%) were intentional self-harm deaths and 14,415 (23%) were assault-related deaths. Since 1999, firearm violence injury death rates have increased by 17%1. Comparatively, traffic-related death rates have decreased by 22%2. In addition to mortality, firearm violence injury exerts an annual burden of over $2.8 billion on the healthcare system3.
Despite the epidemiology, there is a remarkable sense of dissociative academia when it comes to firearm violence injury research. Consequently, the tenants of evidence-based medicine are often superseded by one of two contrasting ideological convictions about firearm ownership. In light of the recent #ThisIsOurLane movement, the narrative from within the healthcare community has been carefully reconstructed to reiterate that firearm violence is a public health problem, not a political one. The American College of Surgeons (ACS) consensus strategy titled “Freedom with Responsibility” predicates that firearm ownership is a Constitutionally protected liberty, and in doing so, highlights violence as the proximate cause to be prevented2. While perceptions at the nexus of healthcare, injury epidemiology, and firearm policy are certainly changing, there is a dearth of conclusive, high-quality evidence available to inform policy and practice4. Under-funding, political jettison, and a history of nonconstructive discourse have all contributed to this shortfall5,6. A recent paper by Sarani et al. in the Journal of American College of Surgeons (JACS) prompts the familiar precedent for objective, evidence-based analysis that future work should emulate7.
The Study
Sarani et al. conducted a retrospective review of 232 autopsy reports from 23 distinct civilian public mass shooting (CPMS) events found in the New York Police Department 2016 Active Shooter Summary Report as well as the US Federal Bureau of Investigation (FBI) report of active shooter events (2000 – 2016). Upon examination of the location of wounds on the body based on firearm type, there was insignificant variability with respect to firearm type. However, wounds to the chest/upper back/extremities were significantly more prevalent than wounds to the head/low back/neck. Fatal injuries to the chest/upper back remained prevalent, but a fatal injury to an extremity was rare. Not surprisingly, the organ injury most often resulting in death was the brain, followed by the lung. However, there was a significant association between firearm type and injury to the brain, with 56% of persons shot with a handgun sustaining a fatal injury to the brain. Among those shot by a firearm, the percentages with fatal (head/abdomen) wounds were classified by shotgun (27%/41%), rifle (29%/11%), multiple firearms (41%/9%), or handgun (58%/15%).
The study concludes that, despite lack of a direct significance of association (attributed to small sample size), events using a handgun were associated with a higher percentage killed, and events using a rifle were associated with more people shot. Therefore, CPMS events carried out with a handgun are more lethal than those associated with the use of a rifle. Additionally, given the rarity of mortality from extremity wounds, future treatment strategy needs to go beyond the use of tourniquets. A holistic approach to the prevention of firearm violence proxies concurrent with resource allocation that aligns with the evidence (in this case, both pistols and rifles posing their own ultimate impacts) is necessary to impact legislative change in this area.
Discussion on the paucity of information regarding details such as bullet characteristics is an unfortunate reality for most facets of firearm violence injury research. Much of the analysis that could not reach statistical significance is potentially “insignificant” due to restricted sample size. Researchers share that state laws or local policy precluding release of autopsy information sequestered 44% of CPMS observations identified. Future work in this area should build on Sarani et al.’s work but remain cognizant of ways to yield more inference from their design. While the use of an expert panel to make the determination of potential preventable death (PPD) allowed researchers to reach consensus, they notably missed out on an opportunity to discuss inter-rater variability (re: Cohen’s kappa coefficient) among experts and their perceptions of survivability given the hindsight of an autopsy report. Additionally, the assigned minimum inter-rater agreement of 80% allowed human subjectivity for analysis of a data set that is otherwise so readily and absolutely dichotomized. For example, rather than a human determination of PPD, a statistically sound approach would have been to utilize Generalized Estimating Equations (GEEs) fit with Odds Ratio (OR) dependence structures to assess covariate effects (e.g., pre-hospital care available within 10 minutes of injury, trauma center care within 1 hour of injury) on determining odds of observing mortality or associated organ injury. Furthermore, bivariate logistic regression specified for each associated organ injury may allow researchers to use specific organ injuries as proxy predictors of outcome, allowing the potential for a priori severity assessment without a context of post hoc prognostication.
References
- Centers for Disease Control and Prevention, National Center for Health Statistics. Underlying Cause of Death. 1999-2016 on CDC WONDER Online Database, released December 2017. Data are from the Multiple Cause of Death Files, 1999-2016, as compiled from data provided by the 57 vital statistics jurisdictions through the Vital Statistics Cooperative Program
- Stewart RM, Kuhls DA, Rotondo MF, Bulger EM. Freedom with Responsibility: A Consensus Strategy for Preventing Injury, Death, and Disability from Firearm Violence. Journal of the American College of Surgeons. 2018;227(2):281-283. doi:10.1016/j.jamcollsurg.2018.04.006
- Gani F, Sakran JV, Canner JK. Emergency Department Visits For Firearm-Related Injuries In The United States, 2006–14. Health Affairs. 2017;36(10):1729-1738. doi:10.1377/hlthaff.2017.0625
- Suicide, Guns, and Why Research Matters. AFFIRM. https://affirmresearch.org/perspectives/suicide-guns-and-why-research-matters/. Published January 10, 2019. Accessed February 3, 2019.
- Jehan F, Pandit V, O’Keeffe T, et al. The burden of firearm violence in the United States: stricter laws result in safer states. Journal of Injury and Violence Research. 2017;10(1). doi:10.5249/jivr.v10i1.951
- The History Behind Gun Violence Injury Research. AFFIRM. https://affirmresearch.org/perspectives/the-history-behind-gun-violence-injury-research/. Published November 28, 2018. Accessed February 3, 2019.
- Sarani B, Hendrix C, Matecki M, et al. Wounding Patterns Based on Firearm Type in Civilian Public Mass Shootings in the United States. Journal of the American College of Surgeons. 2019;228(3):228-234. doi:10.1016/j.jamcollsurg.2018.11.014

Ameer Khalek '18, MPH is a former research assistant for Urgent Matters and a medical student at Touro University Nevada.