When faced with cancer, there are many difficult questions
Who are the best doctors? Where can I get help? Will I get well? But there's no question about where to go: The GW Cancer Center.
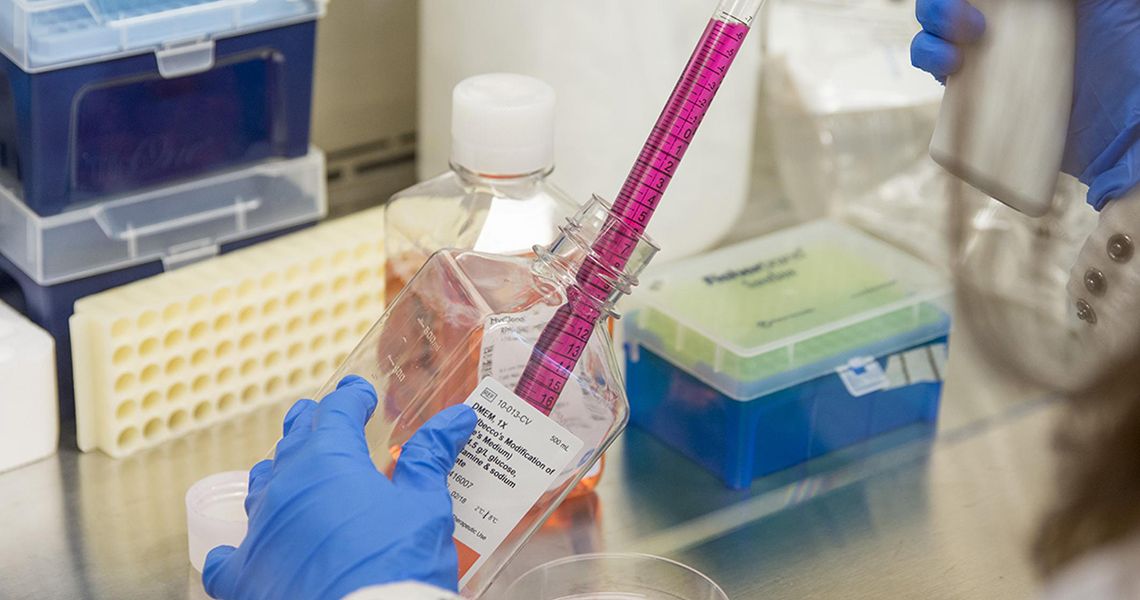
The GW Cancer Center boasts state-of-the-art research facilities dedicated to cancer discovery through interdisciplinary collaboration with scientists and clinicians throughout GW.

We are pleased that you have selected the GW Cancer Center to provide your cancer care and support. The information found here will acquaint you with available information and resources.

The GW Cancer Center provides a comprehensive range of research education and career development programs designed to equip the next generation of scientists and health care providers.
The GW Cancer Center Patient Experience

Joy West
Vocal Cord Cancer
Watch Joy's Video

Jeffrey Gray
Prostate Cancer
Watch Jeffrey's Video

Claudia Acosta
Colon Cancer
Watch Claudia's Video






